



The Supreme Court's Harish Rana judgment confirmed the legality of passive euthanasia and the constitutional Right to Die with Dignity (Article 21). The ruling simplified the procedure for implementing a living will and emphasized the urgent need for Parliament to enact comprehensive end-of-life legislation to ensure ethical clarity, and balance individual autonomy.

Copyright infringement not intended
Picture Courtesy: mathrubhumi
Context
The Supreme Court recently allowed withdrawal of life support for Harish Rana, a man in a permanent vegetative state for about 13 years.
What is Euthanasia?
Euthanasia, meaning "good death," refers to the practice of ending a life to relieve unbearable pain and suffering.
|
Type of Euthanasia |
Description |
Legal Status in India |
|
Active Euthanasia |
Involves a deliberate act to end a life, such as administering a lethal injection. |
Illegal. Treated as a criminal offense under the Bharatiya Nyaya Sanhita (BNS), 2023 (which replaced the Indian Penal Code, 1860). |
|
Passive Euthanasia |
Involves withdrawing or withholding life-sustaining medical treatment (e.g., ventilator support, artificial nutrition), allowing the underlying disease to cause death. |
Legal, subject to strict guidelines laid down by the Supreme Court. |
Legal document where a person specifies their wishes regarding future medical treatment if they become terminally ill or incapacitated and unable to communicate their decisions.
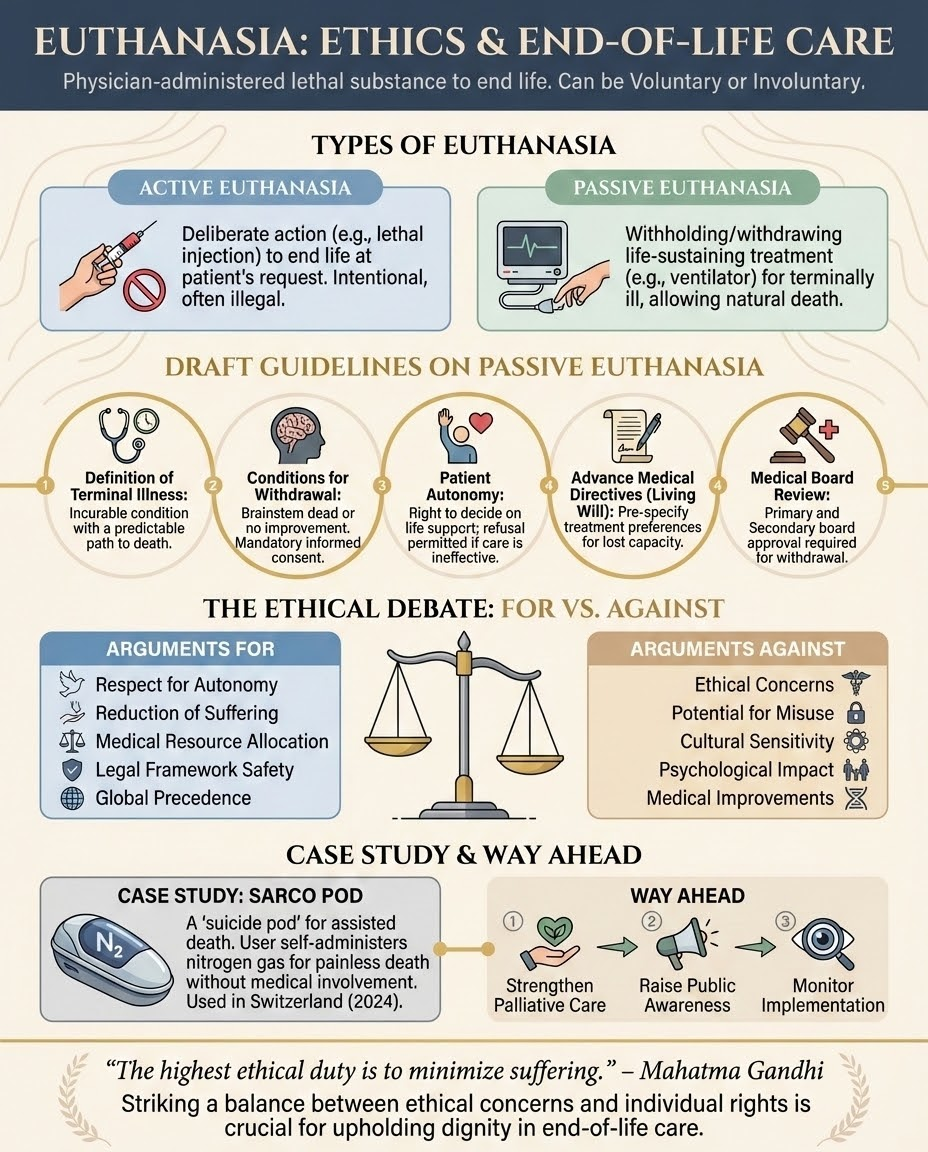
Evolution of the Legal Framework in India
The judiciary has shaped euthanasia stance, interpreting the Right to Life under Article 21 to include the Right to Die with Dignity.
Aruna Shanbaug vs Union of India (2011)
For the first time, the Supreme Court legally recognized passive euthanasia in exceptional circumstances.
It established a stringent procedure requiring the approval of a High Court, which would act under the parens patriae (parent of the nation) principle to protect the patient's best interests.
Common Cause vs Union of India (2018)
Judgment by a five-judge Constitution Bench which declared the "Right to Die with Dignity" as a fundamental right and an integral part of the Right to Life (Article 21).
It legalized Advance Medical Directives (Living Wills) and laid down detailed procedures for their execution and for authorising passive euthanasia.
Modifications to Guidelines (2023)
Acknowledging the procedural difficulties of the 2018 guidelines, the Supreme Court simplified the process.
The modifications introduced clear timelines for medical boards and reduced the role of the Judicial Magistrate to mere intimation, making the process more efficient for families.
Current Procedure for Passive Euthanasia (Post-2023)
Primary Medical Board: The treating hospital forms a board to assess the patient's condition and certify if there is any hope for recovery.
Secondary Medical Board: If the primary board recommends withdrawal, the hospital constitutes a secondary board with independent medical experts to re-examine the patient.
Final Steps: Once both boards agree, the decision is sent to the Judicial Magistrate First Class. The life support can then be withdrawn, ensuring the patient receives palliative care for a comfortable and dignified process.
Socio-Ethical Debate on Euthanasia
Euthanasia debate centers on the conflict between individual autonomy (right to choose death to avoid suffering) and the sanctity of life (duty to preserve life), creating legal and ethical challenges.
Arguments in Favour (Pro-Choice)
Individual Autonomy: Upholds the right of an individual to make decisions about their own body and end-of-life care.
Right to Dignity: Argues that forcing a person to live in a state of constant pain and suffering with no hope of recovery violates their dignity.
Compassion: Seen as a merciful act to relieve a person from intractable suffering.
Arguments Against (Pro-Life)
Sanctity of Life: Based on the moral or religious belief that life is sacred and should not be intentionally ended.
Potential for Misuse: Concerns that vulnerable individuals (elderly, disabled) could be coerced into ending their lives.
Slippery Slope: Fear that legalizing passive euthanasia could eventually lead to the acceptance of active euthanasia.
Physician's Role: Conflicts with the Hippocratic Oath for doctors to "do no harm" and preserve life.
Way Forward
The Supreme Court has emphasized that its guidelines are a temporary fix for a legislative void. A dedicated law passed by Parliament is necessary for several reasons:
Conclusion
Ensuring the right to die with dignity requires a multi-pronged approach: Parliament must enact a comprehensive end-of-life care law, and palliative care infrastructure must be strengthened to provide compassionate, accessible relief from suffering.
Source: INDIANEXPRESS
|
PRACTICE QUESTION Q. A terminally ill patient, who has not left an Advance Directive, is in a state of irreversible coma. The family is divided: one group wants to withdraw life support to end the suffering, while the other insists on continuing treatment. As a member of the Hospital Ethics Committee, what ethical principles would you apply to resolve this deadlock? 20 marks |
Active euthanasia involves a deliberate act to end a person's life, like administering a lethal injection. It is illegal in India and considered culpable homicide. Passive euthanasia involves withdrawing or withholding life-sustaining medical treatment, allowing the person to die from their underlying condition. This is legally permissible in India under strict guidelines set by the Supreme Court.
A 'Living Will', also known as an Advance Medical Directive, was declared legally valid by the Supreme Court in the Common Cause vs Union of India judgment of 2018. This document allows a person to specify their wishes regarding medical treatment for a future time when they may be unable to communicate their decisions.
The primary arguments against euthanasia include the principle of the "sanctity of life," which holds that life should not be ended prematurely. There are also concerns about the potential for misuse and coercion against vulnerable people like the elderly or disabled. Critics also fear a "slippery slope" effect, where legalizing passive euthanasia could eventually lead to the acceptance of active euthanasia.

© 2026 iasgyan. All right reserved