



Antimicrobial Resistance (AMR) occurs when bacteria, viruses, and parasites evolve to resist medicines, making infections harder to treat. Driven by overuse of antibiotics, AMR increases risks of disease spread, severe illness, and death, threatening global public health and modern medicine.

Why In News?
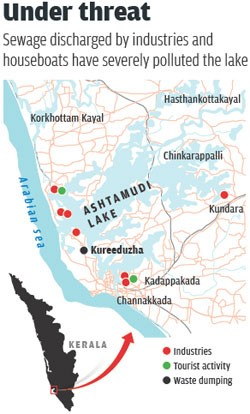
A recent study published in the international journal Environmental and Experimental Biology has identified Ashtamudi Lake in Kerala as a potential hotspot for Antimicrobial Resistance (AMR).
About Ashtamudi Lake
Key Findings of the Study
The study highlighted the presence of bacteria that have evolved mechanisms to survive exposure to potent antibiotics.
What is Antimicrobial Resistance (AMR)?
According to the World Health Organization (WHO), AMR is the resistance acquired by microorganisms against antimicrobial drugs (antibiotics, antivirals, antifungals, and antiparasitics) used to treat infections.
When these pathogens change over time, standard treatments become ineffective, infections persist in the body, and the risk of spread to others increases.
Key Drivers of AMR
The emergence and spread of AMR are fueled by a combination of human, animal, and environmental factors:
Impact of AMR
Human Toll: Bacterial AMR was directly responsible for 1.27 million deaths globally in 2019 and contributed to 4.95 million deaths, according to a Global Research on Antimicrobial Resistance (GRAM) report.
Economic Impact: The World Bank estimates that AMR could cause a global GDP shortfall of up to 3.8% by 2050, potentially pushing 28 million people into extreme poverty.
India's Burden: India faces a high burden due to its large population and high rates of infectious diseases. Over 56,000 newborn deaths annually in India are attributed to sepsis caused by drug-resistant organisms, according to ICMR data.
India's Policy Response
National Action Plan (NAP-AMR): Launched in 2017, the plan follows a "One Health" approach, integrating human, animal, and environmental sectors.
Red Line Campaign: A public awareness initiative requiring a vertical red line on antibiotic packaging to signal they should not be sold or used without a prescription.
Schedule H1: A 2014 amendment to the Drugs and Cosmetics Rules to regulate and restrict the over-the-counter sale of critical antibiotics.
FDC Ban: In 2024, the government banned 156 irrational fixed-dose combination (FDC) drugs, including antibiotic cocktails that lacked scientific justification.
Way Forward
Addressing AMR requires a One Health approach—a collaborative, multisectoral strategy that recognizes the interconnection between the health of people, animals, and the shared environment.
Key priorities include strengthening surveillance through systems like WHO’s GLASS, promoting rational drug use, and investing in the research and development of new vaccines and diagnostic tools.
Source: NEWINDIANEXPRESS
|
PRACTICE QUESTION Q. Antimicrobial Resistance (AMR) is no longer just a clinical challenge but an environmental catastrophe. Discuss. 150 words |
The resistance stems primarily from three anthropogenic sources: inadequate treatment of hospital effluents containing pharmaceutical residues, unregulated use of prophylactic antibiotics in local aquaculture and poultry farming, and untreated sewage discharge into the lake.
Antibiotic residues in water bioaccumulate in seafood. Western markets, like the US and EU, have strict zero-tolerance limits for antibiotic residues. The presence of these residues leads to mass rejections of Indian seafood exports, severely damaging foreign exchange earnings and local coastal livelihoods.
The 'One Health' approach is an integrated framework recognizing that the health of humans, domestic and wild animals, plants, and the wider environment (including ecosystems) are closely linked and interdependent. It requires coordinated action across medical, veterinary, and environmental sectors to combat AMR.



© 2026 iasgyan. All right reserved